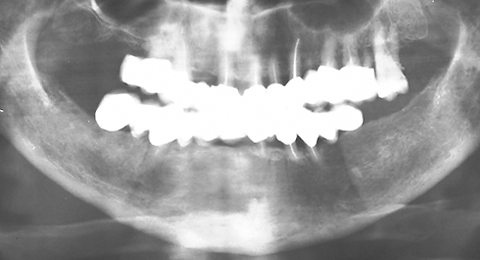
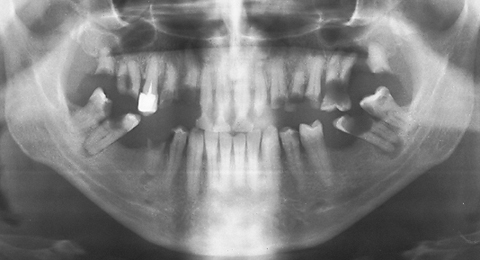
Dental Treatment and Prosthetics Without Implants
When there are teeth missing in the mouth cavity this seriously disturbes the proper bit and chewing harmony. In cases when there are few or inappropriately located teeth to support the bridge construction of the dentures, most commonly removable partial protheses are applyed, but they are widely found as inconvenient. Implants could be used instead, but this requires surgery, and is often too stressing to the patient. The modern solution of the problem is the Attractive Glass Abutment System ZX-27 – an invention, that was given a patent back in 1991.
ZX-27
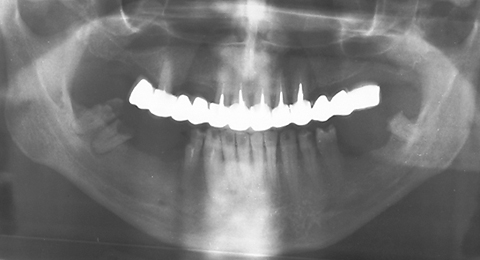
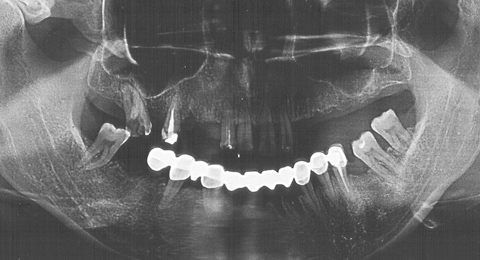
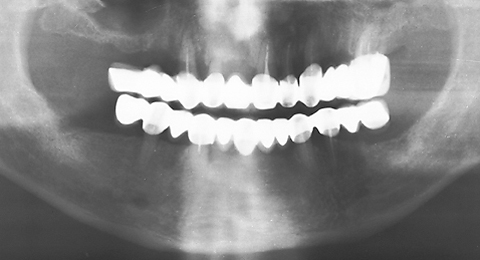
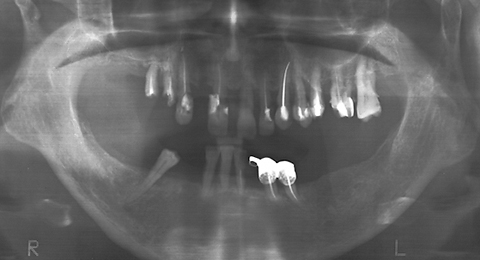
The ZX-27 Attractive Glass Abutment System is a special and unique technique used for building free-end bridges. The key of the system is that the free end of the bridge is supported by a glass abutment made of special material and in a unique way. Patients who still have their own teeth, but prefer not to have prosthetics or implants, or if these cannot be used, may be offered fixed dentures. The ZX-27 system replaces the missing abutment tooth; i.e. a glass abutment is fitted to the gingiva at the critical location. It may also be applied where teeth are missing at one or even both row ends, frontal gaps and combinations of both. Good results can also be achieved in combination with implants.
The Main Characteristics of ZX27 Glass
General glasses did not meet expectations, as dental glasses have to meet many requirements at the same time, namely:
- Meltability
- Workability
- Rigidity
- Chemical resistance
There is no such material amongst general glasses, with the main problems being melt-ability and chemical resistance. General glasses cannot be heat-processed under dental technical conditions. It may fracture during heating invisible hairline-cracks may develop, leading to fracture. Similar processes may occur during cooling. Chemical resistance is another problem. Saliva interacts with the glass and sooner or later evokes chemical reactions. This causes toxic substances such as lead and barium to leach into the saliva from the glass. These substances are harmful to the human organism.
Requirements for suitable glass:
- Workability
- Sufficient rigidity for use
- Chemical resistance and its effect on the organism.
Main characteristics of ZX-27:
- Melting temperature: 1560-1600 °C
- Pressure strength: 120-150 Mpa/kp/mm
- Acid resistance: Hydrolytic Class 1.
- Alkaline solubility: Hydrolytic Class 2.
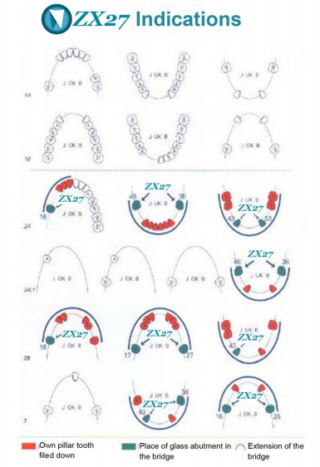
In addition to its main components, ZX-27 contains small amounts of zinc and magnesium but does not contain the harmful substances lead or barium that can be found in general glass and their raw materials. The good workability of ZX-27 glass under laboratory conditions is due to its high boron-trioxide content. That allows the otherwise indispensable high alkaline content to be reduced. Due to the low sodium content, corrosion does not cause local pH rise adjacent to the gum. The above properties assure the suitability of ZX-27 glass in structural dental components.
Examples of indications come from eleven years of practical experience. The use of the abutment is safe alongside conventional technology.
The last ten years and a large number of implantations In many countries have proven that today the glass abutment is widely accepted, despite the previous reservations. This is due to its simplicity and increased convenience for patients. Naturally, several unanswered questions have accompanied my work since its start ten years ago. The first and most important one is that of the general pathological thesis that chronic irritation of non-keratinized mucosa leads to the development of keratinized mucosal epithelium, that is metaplasia, which in turn becomes dysplastic, thus a precancerous condition develops.
Pathological Studies

Cytological smears from mouthwash fluid mainly contained superficial, mature cells. In a sample of 67 cytological specimens from 9 patients with the glass abutment, 17 smears of 3 patients showed a few keratinized but otherwise typical cells besides a large number of non-keratinized epithelial elements (Figure l/a.)
These three patients had bridges supported by two glass abutments built two to four years earlier. There was no significant keratinization either in the specimens of the other patients with glass abutment supported bridges or in the precipitated mouthwash fluid of control patients with traditional bridges.
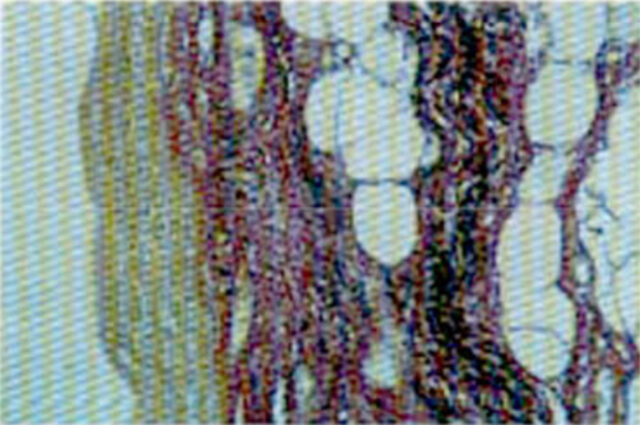
The typical keratinized stratified epithelium was present on the surface of the gum under the glass abutment (figures2/a and 21b). Histologically, the keratinization corresponded to parakeratosis and hyperkeratosis.
There were no mitotic features amongst the epithelial cells and the epithelial layers presented a typical maturation tendency towards the surface (figure 2/a.).



The fixative used poorly preserved tissue glycogen, however, the cytoplasm of the cells contained abundant glycogen (figures 3/a and 31b)
Borders of epithelium and connective tissue were sharp, papillarity was slightly
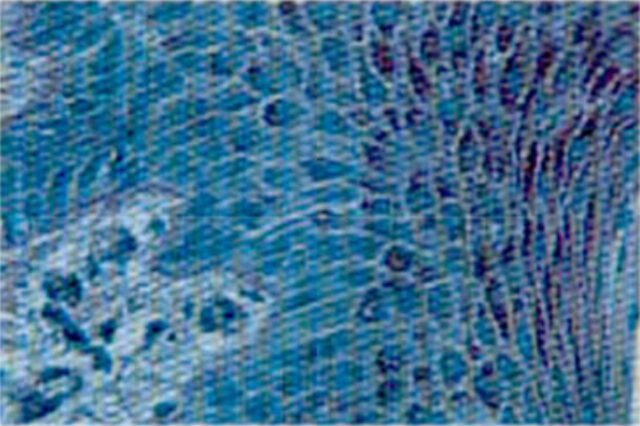 flattened, vascularization was scant but there was an increased amount of collagen (figure 2/a.). The basal layer of the epithelium showed focal, while the spinocellular layer a diffuse and marked expansion (figures 2/a and 21b).
flattened, vascularization was scant but there was an increased amount of collagen (figure 2/a.). The basal layer of the epithelium showed focal, while the spinocellular layer a diffuse and marked expansion (figures 2/a and 21b).
In the gingival tissue from underneath the removable prostheses or from samples without any dentures that served as a control, a tendency to keratinize was also noticed, although the keratinized layer appeared thinner compared to those under the glass abutment (figure 4).
 In scanning using electron microscopy, the surface of the new abutment at the gingival side was smooth. No abrasion, mechanical damage, or deformations as a result of mucosal irritation were found. The elemental composition measured at five different sites (areas of 350-micron diameter) was practically the same. The surface and the chemical composition of the glass abutments implanted between eight and twelve months earlier were equal to that of new abutments.
In scanning using electron microscopy, the surface of the new abutment at the gingival side was smooth. No abrasion, mechanical damage, or deformations as a result of mucosal irritation were found. The elemental composition measured at five different sites (areas of 350-micron diameter) was practically the same. The surface and the chemical composition of the glass abutments implanted between eight and twelve months earlier were equal to that of new abutments.
From these cytological and histological studies, it can be established, that the mucosa under the glass abutment showed a mild but typical keratinous tendency that was characterized as hyperkeratosis and parakeratosis, and not as dysplasia of the precarcinomatous leukoplakia type.
Similar to the mucosa at conventional bridges and removable prostheses used as controls and from patients who chew on the gums, histological findings found harmless, adaptive keratinization. The degree of keratinization was far below that of the leukoplakia noticed due to hot and spicy foods and the cells remained typical.
In conclusion, it can be stated that cytological and histological changes of the mucosa underneath the glass abutment are not different in quality, only in quantity, from those noticed underneath conventional bridges, prostheses, or from those patients without dentures and who chew on their gums.
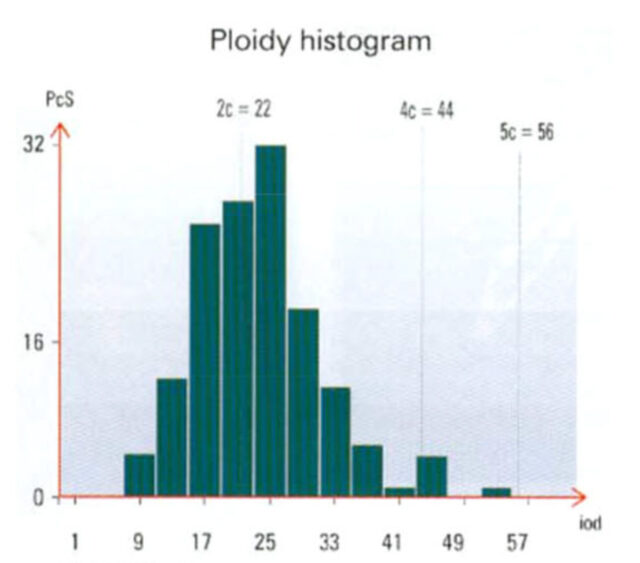
DNA analysis was performed on Feulgen-Schiff specimens by means of a computer-assisted into logical image analysis program (DNASK). This program is able to determine 13 morphometric and densitometric parameters of the nucleus. The image analysis for DNA measurements within the basal cells of the epithelium of the three studied groups (with glass abutments, with removable prostheses, chewing on the gum) revealed normal distribution with a peak at the normal diploid DNA range. The number of tetraploid nuclei remained below 4 % and aneuploid polyploidy did not occur.
DNA analysis is useful in this research as morphologically identical tissue lesions can represent different prognoses if
the cellular DNA content appears changed as determined either by the naked eye or by microscopic examination. These changes can be the result of overloading when the DNA content doubles and polypoid tetraploid cells develop. However, when the epithelium displays a tendency for dysplastic metaplastic changes, which is a pre-cancerous stage, the DNA content not only doubles but changes irregularly and thus can be two and a half fold, threefold or, three and a half fold more than normal. The results of DNA analysis indicated normal diploid tissue appearance in addition to a significantly lower tetraploid cell population as would be due to mechanical stress. We did not find aneuploid polyploidy that characterizes a pre-cancerous stage (figure 5).
Summarizing the results of pathological studies, instead of the expected metaplastic and dysplastic changes that could be reasonably expected from our general pathological knowledge, we found simple adaptive hyperkeratosis underneath the glass abutment, the degree of which did not even reach the degree of hyperkeratosis in patients who chewed on their gums. Glass abutments did not even cause mucosal stress, as was caused by chewing on the gum mucosa.
Static Analysis
For the substitution of so-called free-end situations, the use of removable, anchored, or supported bridgework is recommended by conventional textbook therapeutic indications. The use of removable dentures is often a result of patients’ aversion against these types of prosthetics, or due to biological or financial reasons, or patients’ fear of surgical intervention in case of implantation.
The aim of our static analysis was to verify the importance and role of glass abutments for support and their function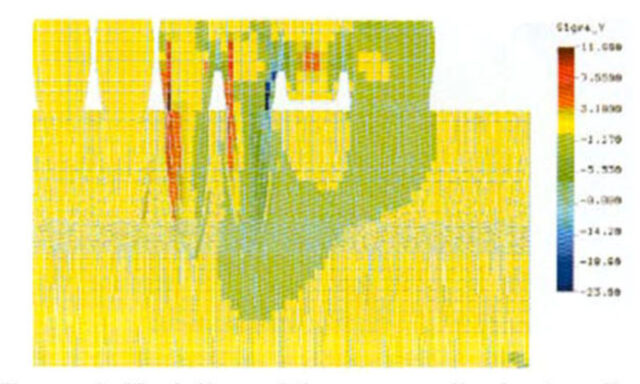 in transmitting the resulting forces. Furthermore, we aimed to contradict the presumption that ZX-27 did not at all differ statically or functionally from conventional free-end bridges. The Transient Element Method used in the study is capable of answering all envisaged and expected questions. Even at first glance, it becomes obvious from the figures that the greatest significance of the glass abutment is the transfer of forces to supporting teeth and thus a relief role (figure 6).
in transmitting the resulting forces. Furthermore, we aimed to contradict the presumption that ZX-27 did not at all differ statically or functionally from conventional free-end bridges. The Transient Element Method used in the study is capable of answering all envisaged and expected questions. Even at first glance, it becomes obvious from the figures that the greatest significance of the glass abutment is the transfer of forces to supporting teeth and thus a relief role (figure 6).
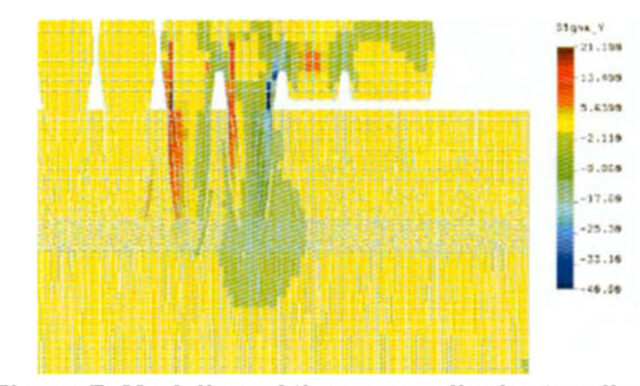
Figure 6. demonstrates well that glass abutments are able to transmit the resulting force much better onto the two supporting teeth than free-end bridges (figures 6-7).
The results of static analyses performed using the Transient Element Method demonstrate that prostheses of glass abutment supports do not follow the established practical and theoretical system of the free-end bridges.
 Although the data in technical literature was determined by data published in the most recent issues of international journals and by our measured data, the accuracy of the calculations was limited by the computing power of the PCs used and by simplifications due to the assumed negligible effect of certain geometric characteristics.
Although the data in technical literature was determined by data published in the most recent issues of international journals and by our measured data, the accuracy of the calculations was limited by the computing power of the PCs used and by simplifications due to the assumed negligible effect of certain geometric characteristics.
The following results were observed:
- gingiva is 2 mm thick
- cortical bone is 3.3 mm thick
- periodontium along the root is 0.25 mm thick
- the thickness of cortical bone is 0.5 mm
The remaining data was easier to obtain due to the comparatively simpler and more accurate measurability of substance specificity. Such specificity includes the metals and ceramics used during fabrication of bridges, and is summarized in a table expressible by Rugalmassi modules and by a so-called Poisson number. Due to the absence of data in the technical literature and as the continually changing, individually derived, personal characteristics are lacking, measurements may contain inaccuracies. However, these results are below the presumed values of real data. This means that oral glass abutment would present better results if we could measure or model them. It so happens that in the case of vertical and lateral forces, the
support provided by concave surfaced glass abutments is more favorable in reality (as characterized by lower equivalent stress) compared to the model calculations of the present plain glass surface (figures 8-9). Concave surface can transmit a lower proportion of lateral force to the convex gum surface, thus decreasing the lateral bending force of the crown (figures 10-11). Consequently this study was, for example, not able to model the effect of pulsating forces on paradental fibers, mucosabone, bed, etc. These effects were supported by further, mainly clinical, longitudinal experiments that will be presented later. Evaluation of the results was difficult as we were unable to obtain records of such measurements in relation to individual dentures. Here I mainly consider the effect of the effect of resulting forces on the paradentium of existing teeth and the measured results in case of model-casted metal plates with partial uni or bilateral anchoring.
After the pathological and static examinations, aimed at answering questions that previously had challenged the suitability of the ZX-27 Attractive Glass Abutment system, had provided reassuring results and chronic toxicity, cytotoxic, genotoxic and bio persistency studies had presented negative results, it became necessary to examine what changes the permanent equipment caused on the bone bed in contact with the surface.